- CANCER CARE
- Cancer Centers of Excellence
- Cancers We Treat
- Brain/Neuro Cancer
- Breast Cancer
- Colorectal Cancer
- Lung Cancer
- Prostate Cancer
- Bile Duct Cancer
- Bladder Cancer
- Bone Cancer
- Cervical Cancer
- Duodenal Cancer
- Esophageal Cancer
- Gallbladder Cancer
- Head and Neck Cancer
- Kidney Cancer
- Leukemia
- Liver Cancer
- Melanoma
- Multiple Myeloma
- Lymphoma
- Ovarian Cancer
- Pancreatic Cancer
- Rectal Cancer
- Soft Tissue/Sarcoma
- Small Intestine Cancer
- Stomach Cancer
- Thyroid Cancer
- Uterine Cancer
- Vaginal Cancer
- Vulvar Cancer
- Testicular Cancer
- Cancer Treatment Options
- Cancer Support Services
- Fertility Program
- Nurse/Patient Navigators
- Nutrition Counseling
- Supportive Care and Services
- Lymphedema Management Program
- Quit Smoking Program
- Oncology Social Work
- Support Groups
- Survivorship Program
- Wellness Programs
- Community Resources
- Lung Navigation Program
- Breast Health Navigation Program
- Gastrointestinal (GI) Cancer Navigation Program
- Gynecological Oncology Navigation Program
- Hospice Service
- Cancer Genetics Program
- Cancer Centers of Excellence
- Cancers We Treat
- Brain/Neuro Cancer
- Breast Cancer
- Colorectal Cancer
- Lung Cancer
- Prostate Cancer
- Bile Duct Cancer
- Bladder Cancer
- Bone Cancer
- Cervical Cancer
- Duodenal Cancer
- Esophageal Cancer
- Gallbladder Cancer
- Head and Neck Cancer
- Kidney Cancer
- Leukemia
- Liver Cancer
- Melanoma
- Multiple Myeloma
- Lymphoma
- Ovarian Cancer
- Pancreatic Cancer
- Rectal Cancer
- Soft Tissue/Sarcoma
- Small Intestine Cancer
- Stomach Cancer
- Thyroid Cancer
- Uterine Cancer
- Vaginal Cancer
- Vulvar Cancer
- Testicular Cancer
- Cancer Treatment Options
- Cancer Support Services
- Fertility Program
- Nurse/Patient Navigators
- Nutrition Counseling
- Supportive Care and Services
- Lymphedema Management Program
- Quit Smoking Program
- Oncology Social Work
- Support Groups
- Survivorship Program
- Wellness Programs
- Community Resources
- Lung Navigation Program
- Breast Health Navigation Program
- Gastrointestinal (GI) Cancer Navigation Program
- Gynecological Oncology Navigation Program
- Hospice Service
- Cancer Genetics Program
What is Radiation Oncology?
Radiation oncology treatments focus on using radiation to treat cancer by directing high-energy beams at cancer cells. The goal is to destroy the problem cells and keep them from dividing and multiplying, while avoiding the healthy surrounding cells, resulting in better patient outcomes.
Why Capital Health Radiation Oncology?
Capital Health’s radiation oncology team is made up of some of the best cancer experts in the area to provide you, our patient, the highest level of cancer care available.

- Accredited by the American College of Radiology
- Leading Edge Technology to enhance the expert technique and treatment of cancer.
- Combining technologies such as the TrueBeam™ Linear Accelerator, CyberKnife® Robotic Radiosurgery System, Vision RT surface treatment and Varian HDR Brachytherapy system, Capital Health is proud to have the most advanced radiation devices under one roof to provide comprehensive, efficient treatment plans for patients.
How is Radiation Oncology Used in Cancer Treatment?
Capital Health offers multiple types of radiation treatments. You might receive one or more of these treatments depending on your cancer type, location, and severity:
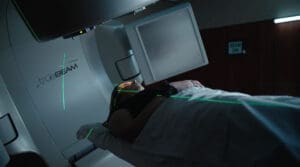

- TrueBeam™ Linear Accelerator provides physicians the ability to manage challenging cancers with unparalleled ease and precision anywhere in the body from nearly any angle.
- CyberKnife® Robotic Radiosurgery System – available at Capital Health since 2007, CyberKnife® is a non-invasive procedure used to treat tumors—benign and cancerous. Radiation beams can be sculpted to reach small, deeply imbedded, complex masses. There are no incisions whatsoever.
- High Dose Rate (HDR) Brachytherapy
- Surface Guided Radiation Treatment with Respiratory Gating, also known as Deep Inspiration Breath Hold (DIBH)
- Nuclear Medicine uses radioactive drugs to identify cancer cells. The radioactive liquid is injected into the veins where it travels through the body and attaches itself to tumor cells. When the drug attaches to the cells, it then attacks the cancer cells with radiation, causing them to die.
The Radiation Oncology Process
The radiation oncology process at Capital Health is about more than just the advanced treatment. It’s a promise from our team to be there with you step-by-step through this journey, from start to finish.


- Consultation: In your initial meeting, you’ll meet your nurses and doctors, and undergo a physical exam. Your care team will walk you through everything you need to know about radiation and the treatment options for your diagnosis.
- CT Scan: Prior to your radiation treatment, you’ll have a CT scan of your body with a focus on the proposed treatment site. Your team will take photographs and may give you treatment tattoos, which allow them to line up radiation treatments accurately. The simulation CT scans are what each of our physicians use to identify and outline, or contour, the areas for treatment. Prior to your CT scan, your care team may recommend additional prep, such as a special diet, placement of fiducials, etc.
- Treatment Planning: Once CT scans are loaded and areas are identified and contoured for treatment, a treatment plan is created by our dosimetrists or physicists.
- Initial Treatment: At this stage, your treatment begins. Your care team will check X-ray films or CT scans to verify the appropriate treatment site. Then, once a second check on the treatment plan is done by our multidisciplinary cancer team, the first treatment will be administered.
- Daily Treatments: Patients may have films such as x-rays or CT scans before treatments, or just setup by tattoos, fiducials, masks, surface images, etc.
- Weekly Visits: Your doctor will evaluate the progress of your treatment weekly and will evaluate and manage any side effects.
- Support Along the Way: As our patient we want you to be sure we’re thinking about supporting you in ways that go beyond just treatment, so we offer the following areas of support:
- Dietary: You will meet with a dietitian just once, or weekly as needed to ensure you’re getting the nutrients you need during treatment
- Social Services: All patients have the option to meet with a social worker upon request
- Financial: All patients are paired with a financial navigator to make sense of the billing and insurance
- Additional Support: In addition, we offer support services such as palliative care, speech therapy, site-specific navigators (as needed), fertility programs, rehab, and more
Concierge Services:
At Capital Health Radiation Oncology, the patient is at the center of everything we do.
That’s why we go above and beyond to provide you with anything you might need through our concierge services:
- Free transportation to daily appointments
- Parking outside the cancer center door
- Location close to the spa/front entrance
- On-site registration available within our department to assist with scheduling of additional services
- Assistance with all appointment scheduling on-site, within our department
- All support staff physically located within the Radiation Oncology space:
- Navigators located on-site in our department
- Dietitians meet with all patients
- Social worker on-site when needed
- Speech therapists for swallow studies
- Celebratory gong, as well as a photo op and poem reading upon completion of treatment
What are some of the therapies I might expect?
Stereotactic radiosurgery (SRS) uses 3-dimensional imaging and computer guidance to shape and deliver radiation beams with pinpoint accuracy to tumors without damaging the surrounding healthy tissue.

